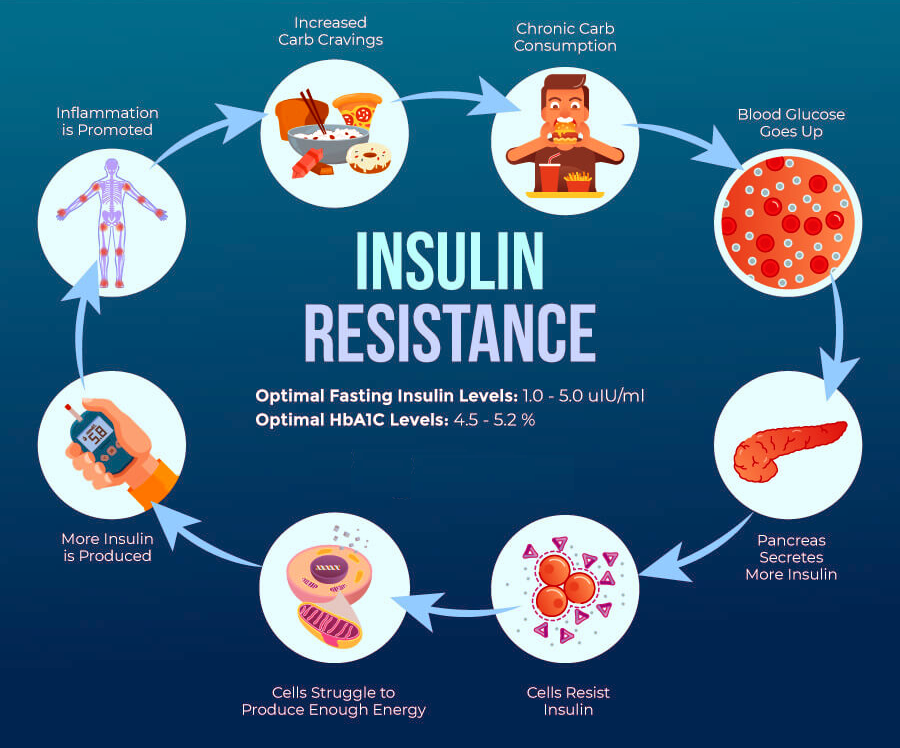
Insulin resistance is a condition where the body’s cells become resistant to insulin, a hormone that helps regulate blood sugar levels. When cells become insulin resistant, they no longer respond as effectively to insulin, and the body needs to produce more insulin to keep blood sugar levels under control. Over time, this can lead to high blood sugar levels, which can cause a range of health problems, including type 2 diabetes.
Insulin resistance can be caused by a number of factors, including genetics, diet, lack of exercise, and obesity. When the body is exposed to high levels of insulin for a long period of time, as is the case in people with insulin resistance, it can lead to chronic inflammation.
Chronic inflammation occurs when the body’s immune system becomes activated and stays activated for long periods of time. This can lead to damage to tissues and organs throughout the body, including the liver, pancreas, and heart. Inflammation is also a key driver of many chronic diseases, including type 2 diabetes, cardiovascular disease, and certain types of cancer.
Insulin resistance can affect a number of organs throughout the body, including the liver, pancreas, and skeletal muscle. In the liver, insulin resistance can lead to the development of non-alcoholic fatty liver disease (NAFLD), a condition in which fat accumulates in the liver. Over time, this can lead to inflammation and scarring of the liver, which can eventually lead to liver failure.
In the pancreas, insulin resistance can lead to the development of type 2 diabetes. When the pancreas becomes unable to produce enough insulin to keep up with the body’s demands, blood sugar levels can rise, leading to the development of diabetes.
In skeletal muscle, insulin resistance can lead to decreased glucose uptake and utilization, which can lead to muscle wasting and weakness. This can also lead to the development of metabolic disorders, such as metabolic syndrome.
And …. The BIG one, the brain
Inflammation can have a significant impact on the brain and can contribute to various neurological and psychiatric disorders. When the immune system is activated, pro-inflammatory cytokines are released, which can cross the blood-brain barrier and cause inflammation in the brain. This can lead to a number of changes in brain function, including alterations in neurotransmitter systems, changes in neural plasticity, and neurodegeneration.
One of the most well-known effects of inflammation on the brain is the development of depression. Studies have found that individuals with depression have higher levels of pro-inflammatory cytokines in their blood and cerebrospinal fluid than non-depressed individuals. These cytokines can affect the production and availability of neurotransmitters like serotonin and dopamine, which are crucial for regulating mood.
Inflammation has also been linked to the development of other neurological disorders, such as Alzheimer’s disease and Parkinson’s disease. Chronic inflammation can contribute to the accumulation of beta-amyloid plaques and neurofibrillary tangles in the brain, which are hallmarks of Alzheimer’s disease. Similarly, inflammation can lead to the degeneration of dopamine-producing neurons in the substantia nigra, which is a key characteristic of Parkinson’s disease.
Furthermore, inflammation can also affect cognitive function, including attention, memory, and decision-making. Chronic inflammation can impair neural plasticity and lead to the loss of synaptic connections in the brain, which can contribute to cognitive decline. Inflammation may also play a role in the development of conditions like schizophrenia, which is associated with alterations in immune system function.
In conclusion, inflammation can have significant effects on the brain and contribute to the development of a variety of neurological and psychiatric disorders. The immune system plays a complex role in the regulation of brain function, and dysregulation of this system can have far-reaching consequences. Further research is needed to better understand the mechanisms underlying inflammation-related changes in the brain and to develop effective treatments for these conditions.
While insulin resistance can be a serious health condition, it is possible to reduce the inflammation associated with it through changes to diet and lifestyle. One approach that has shown promise in reducing inflammation and reversing insulin resistance is the ketogenic diet.
The ketogenic diet is a high-fat, low-carbohydrate diet that is designed to shift the body’s metabolism away from glucose and towards ketones, which are produced when the body breaks down fat. By reducing the amount of glucose in the body, the ketogenic diet can help to reduce the insulin resistance that is associated with chronic inflammation.
Similarly, the carnivore diet is a high-protein, high-fat, and very low-carbohydrate diet that eliminates all plant-based foods. This diet is thought to help reduce inflammation by eliminating foods that may be triggering an immune response in the body.
Both the ketogenic and carnivore diets have been shown to be effective in reducing inflammation and improving insulin resistance in some people.
Insulin resistance is a serious health condition that can lead to chronic inflammation and damage to organs throughout the body. The ketogenic and carnivore diets are two approaches that have shown promise in reducing inflammation and improving insulin resistance. There are more areas in the body that are negatively impacted by insulin resistance, Above is not a complete list by any means, yet it should bring about the desired result where after viewing this article, the reader will be curious enough regarding this overwhelming, nationwide health problem and seek further information by researching on their own.
- Henson, D. A., et al. “Chronic Inflammation in Insulin Resistance: A Review of the Adverse Effects of Inflammation on Insulin Sensitivity, β-Cell Function, and Glycemic Control.” Advances in Nutrition, vol. 8, no. 5, 2017, pp. 644–655. doi: 10.3945/an.117.015132. (https://academic.oup.com/advances/article/8/5/644/4558119)
- Kim, Y. S., et al. “The Role of Chronic Low-Grade Inflammation in the Development of Insulin Resistance and Obesity.” Korean Journal of Internal Medicine, vol. 28, no. 6, 2013, pp. 672–677. doi: 10.3904/kjim.2013.28.6.672. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3832466/)
- Volek, J. S., and S. D. Phinney. “The Art and Science of Low Carbohydrate Living: An Expert Guide to Making the Life-Saving Benefits of Carbohydrate Restriction Sustainable and Enjoyable.” Beyond Obesity LLC, 2011. (https://www.amazon.com/Art-Science-Low-Carbohydrate-Living/dp/0983490708)
- Gershuni, V. M., et al. “Ketogenic Diet: What Is the Evidence?” The Physician and Sportsmedicine, vol. 47, no. 1, 2019, pp. 20–26. doi: 10.1080/00913847.2018.1548791. (https://www.tandfonline.com/doi/full/10.1080/00913847.2018.1548791)
- Klement, R. J. “The Role of a Ketogenic Diet in Cancer Therapy.” Current Opinion in Pharmacology, vol. 13, no. 4, 2013, pp. 530–535. doi: 10.1016/j.coph.2013.05.008. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3894518/)
- Eaton, S. B., et al. “The Ancestral Human Diet: What Was It and Should It Be a Paradigm for Contemporary Nutrition?” Proceedings of the Nutrition Society, vol. 65, no. 1, 2006, pp. 1–6. doi: 10.1079/PNS2005471. (https://www.cambridge.org/core/journals/proceedings-of-the-nutrition-society/article/ancestral-human-diet-what-was-it-and-should-it-be-a-paradigm-for-contemporary-nutrition/596CA2AA59D8FD6E5E7DFDE6FF9A5B5B)
Visit the following link for testimonial stories from almost 1000 people that have reversed many metabolic diseases by eating a Carnivorous or Keto diet. More stories like these are being told every day.